How do Indians reduce visceral belly fat? Indians often carry dangerous visceral fat at low BMI, the thin-fat phenotype. Effective belly fat reduction requires a waist-circumference target of under 90 cm in men and 80 cm in women, a high-protein muscle-preserving plan, resistance training, and, where indicated, supervised GLP-1 therapy. Crash diets shrink muscle, not visceral fat. Physician-led protocols work.
The DermaVue Clinics medical team treats belly fat in Indians as a visceral fat problem, not a cosmetic one. The protocol combines waist circumference monitoring, body composition analysis, a 1.2 to 1.6 g/kg protein target, structured resistance training, and GLP-1 receptor agonist therapy when clinically indicated. The approach is built around the South Asian thin-fat phenotype, where visceral fat is high even at normal BMI. Across 7 physician-led DermaVue centres in Kerala and Tamil Nadu, the team has supported a patient base reflected in 7,200 plus reviews with a 4.8 average star rating.
Why Your Belly Fat Won't Go Away (No Matter What You Try)
You've tried intermittent fasting, keto, walking 10,000 steps, and green tea. Your arms got thinner. Your face got leaner. But your belly? It didn't move. Here's why this keeps happening to you.
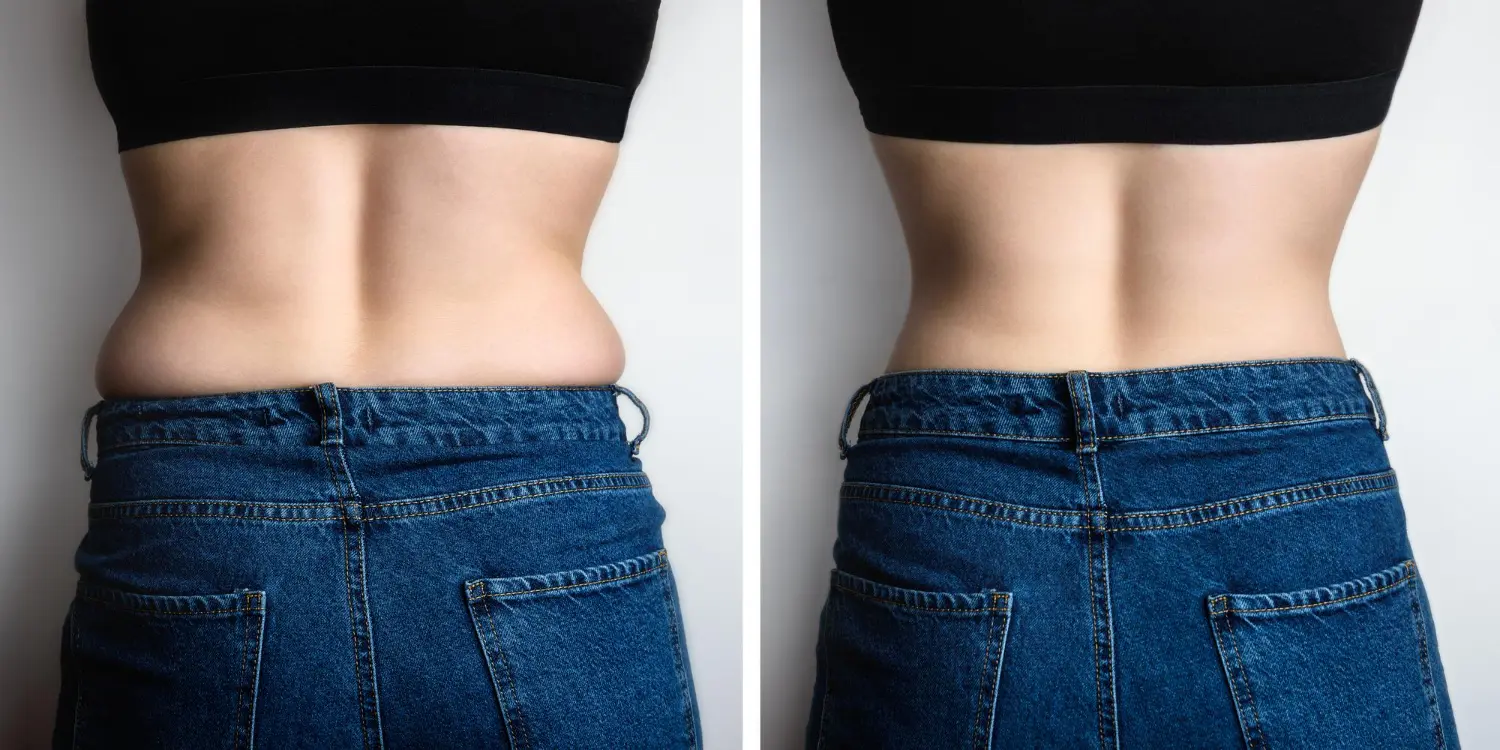
What is Visceral Fat? (And Why It's Dangerous for Indians)
Not all fat is created equal. The fat you can pinch is subcutaneous fat. Annoying but mostly harmless. The fat you can't see is visceral fat. And it's actively damaging your health from the inside.

| Factor | Subcutaneous Fat | Visceral Fat |
|---|---|---|
| Location | Just under the skin | Around liver, pancreas, intestines |
| Visibility | You can pinch it | Hidden. Hard belly, not soft |
| Danger Level | Low | High |
| Response to Dieting | Responds to calorie deficit | Resistant. Needs medical intervention |
Why Visceral Fat is Deadly
ICD-10 E66.01 Central Obesity.
Per Lancet research on Asian Indian fat distribution.
Month 6 interim: 10 to 16% total weight reduction.
The 'Thin-Fat Indian' Phenotype Explained
Research published in The Lancet shows that Indian bodies store fat differently. Two doctors with the exact same BMI can have dramatically different body fat percentages. And dramatically different health risks.
| Measurement | Indian Doctor | European Doctor |
|---|---|---|
| BMI | 22.3 kg/m² | 22.3 kg/m² |
| Body Fat % | 21.2% | 9.1% |
| Visceral Fat | High | Normal |
| Health Risk | Elevated | Low |
Expected Results Timeline
| Timeframe | Expected Result |
|---|---|
| Month 1 | Reduced appetite, early weight change 1-3 kg |
| Month 3 | Visible waist reduction, 5-8 cm lost |
| Month 6 | 10-16% total weight loss, significant visceral fat loss |
| Month 12 | 15-22% total weight loss, metabolic improvement confirmed by labs |
Why Belly Fat Requires Medical Treatment
Diet Alone Fails
Calorie restriction causes indiscriminate weight loss. You lose muscle and subcutaneous fat, but visceral fat is metabolically resistant and the last to go. Most people quit before reaching it.
Cardio Alone Fails
Running and cycling burn calories but don't specifically target visceral fat. Without resistance training, you lose muscle mass. Which lowers your metabolism and makes the belly worse long-term.
Supplements & Detox Fail
No supplement, tea, or "detox" product has evidence for visceral fat reduction. These products target your wallet, not your belly fat. Medical intervention with proven GLP-1 therapy is the evidence-based approach.
How DermaVue Treats Visceral Fat. The 6-Step Protocol
Body Composition Analysis
Waist circumference measurement and bioelectrical impedance analysis (BIA/InBody scan) to quantify your visceral fat level, lean muscle mass, and body water percentage.
Metabolic Lab Panel
HOMA-IR (insulin resistance score), HbA1c (3-month blood sugar average), fasting insulin, lipid profile, liver function, and thyroid panel to identify metabolic dysfunction.
GLP-1 Therapy Selection
Dermatologist selects the appropriate GLP-1 receptor agonist (semaglutide or tirzepatide) based on your metabolic profile, with gradual dose titration for tolerability.
Dietitian-Led Nutrition Plan
Protein-optimized meal plan (1.2-1.6g protein per kg body weight) designed by our clinical dietitian. Vegetarian and non-vegetarian options with Indian meal frameworks. See our detailed diet plan guide.
Resistance Training Protocol
Structured strength training program to preserve lean muscle mass during weight loss. Progressive overload principles with exercises achievable at any fitness level. See our exercise plan guide.
Monthly Monitoring + Face-Saver Dermatology
Monthly body composition scans, lab retesting at 3-month intervals, and dermatology support for skin changes during weight loss. Including facial volume loss prevention.
The Muscle Preservation Challenge
Without proper supervision, 25-45% of GLP-1 weight loss can be lean muscle mass. This is called sarcopenic obesity. You lose weight on the scale but become weaker, slower, and more metabolically fragile.
DermaVue's Sarcopenia Prevention Protocol
Protein Optimization
1.2-1.6g protein per kg body weight daily. Meal timing around training. Vegetarian-friendly plans with paneer, dal, soya, and supplementation.
Creatine Supplementation
3-5g creatine monohydrate daily. The most researched supplement for muscle preservation during caloric deficit. Safe, effective, and affordable.
Resistance Training
Progressive overload strength training 3x per week. Compound movements prioritized. No gym experience needed. We start from scratch.
Grip Strength Monitoring
Monthly dynamometer testing to track muscle function. Grip strength is the single best predictor of overall muscle health and sarcopenia risk.
Who Is This Treatment For?
The belly fat reduction program is designed for Indian adults who carry excess visceral fat despite appearing normal weight. You may be an ideal candidate if:
Thin-fat phenotype: Normal BMI (18.5-24.9) but elevated body fat percentage with visible belly
Central obesity: Waist circumference >85 cm (men) or >75 cm (women) per ICMR guidelines
Pre-diabetes: Fasting glucose 100-125 mg/dL or HbA1c 5.7-6.4% with abdominal fat
PCOS with belly fat: Polycystic ovary syndrome with central fat deposition and insulin resistance
Metabolic syndrome: Elevated triglycerides, low HDL, raised fasting glucose despite appearing lean
Diet-resistant belly: Stubborn abdominal fat that persists despite calorie restriction and regular physical activity
Visceral Belly Fat: The Indian Phenotype Problem
Indian bodies store fat in the wrong place. Even at a normal BMI by international standards, South Asians carry significantly more fat around the liver, pancreas, and intestines than matched European populations. This is the visceral belly fat problem and it is the central reason Indian patients develop diabetes, fatty liver, and heart disease at lower body weights than the rest of the world.
The Asian Indian Consensus Statement set the diagnostic floor for abdominal obesity at 90 cm waist for men and 80 cm waist for women, well below the 102 cm and 88 cm cutoffs used in Western populations [Misra A et al. JAPI 2009]. The same consensus moved overweight to BMI 23 and obese to BMI 25 for Asian Indians. If you measure your waist at navel level and you cross those numbers, you are inside the at-risk band, regardless of how the scale reads.
The downstream signal is real. The ICMR-INDIAB-17 study found type 2 diabetes prevalence in Kerala at 19.4 percent, the highest of any Indian state, with another 18 percent of Kerala adults sitting in the prediabetes range [Anjana RM et al. ICMR-INDIAB-17, Lancet D&E 2023]. That is not a coincidence. It is what happens when a population with a visceral fat phenotype meets a high refined carbohydrate diet and a sedentary lifestyle. Visceral fat is the metabolic engine driving all of it.
The clinical case for treating visceral fat as a cardiovascular target was strengthened by the SELECT trial, which showed that semaglutide produced a 20 percent reduction in major adverse cardiovascular events in patients with established cardiovascular disease and obesity, even without diabetes [Lincoff AM et al. SELECT, NEJM 2023]. The implication for the Indian patient is direct. Visceral fat is not cosmetic. Reducing it meaningfully reduces cardiovascular risk.
NAFLD and Belly Fat: The Kerala Connection
Non-alcoholic fatty liver disease, now reclassified as MASLD (metabolic dysfunction associated steatotic liver disease), is the silent partner of visceral belly fat. Fat that should sit in subcutaneous depots gets pushed into the liver and pancreas. The liver becomes mildly inflamed, ALT and AST creep up, and over years a fraction of patients move into fibrosis and cirrhosis. Most patients have no symptoms until the disease is already advanced.
Kerala sits at the high end of the curve for two reasons. First, the Asian Indian phenotype favours visceral and hepatic fat deposition. Second, ICMR-INDIAB-17 placed Kerala T2D prevalence at 19.4 percent, and fatty liver tracks closely with diabetes and prediabetes [Anjana RM et al. ICMR-INDIAB-17, Lancet D&E 2023]. Hospital series across Kerala suggest fatty liver prevalence in the adult outpatient population north of 30 percent, including thin patients with central obesity.
At DermaVue we screen for fatty liver as part of the belly fat workup. The baseline is a liver function test (ALT, AST, GGT, bilirubin, albumin) plus a fasting lipid panel. When ALT is elevated, central obesity is present, or HOMA-IR is high, we refer for FibroScan transient elastography to quantify liver stiffness and steatosis. FibroScan is a 10 minute non-invasive bedside scan available at most major Kerala hospitals. The result tells us whether we are looking at simple steatosis or whether fibrosis has begun. Treatment is structural. Visceral fat reduction through GLP-1 therapy, dietary change, and resistance training is the most effective intervention available outside a hepatology unit.
Body Composition: DEXA and InBody
Scale weight lies. Two patients at 75 kg can have completely different bodies. One can carry 20 kg of muscle and 15 kg of fat. The other can carry 12 kg of muscle and 25 kg of fat. The scale calls them identical. The metabolic risk profile is not.
DermaVue tracks fat mass, lean mass, visceral fat rating, and skeletal muscle index separately at every visit. The first-line tool in the clinic is InBody bioelectrical impedance analysis, a 30 second test that estimates segmental muscle and fat distribution and tracks change over time. For patients with complex metabolic disease or sarcopenic obesity, we refer for DEXA (dual energy X-ray absorptiometry) at partner imaging centres in Kochi, Kollam, and Coimbatore. DEXA is the gold standard for body composition and gives a clean read on visceral fat area, regional fat, and lean mass with a one percent margin of error. The dose of radiation is roughly the same as a transcontinental flight.
The point is simple. We do not care if your scale moves down by 8 kg if 4 kg of that came from muscle. The goal of the program is fat loss, not weight loss. Body composition data is what allows us to tell the difference, dose the protein target correctly, and dial the resistance training plan up or down at every monthly review.
Belly Fat in Women: Hormonal Causes
A woman's belly fat pattern is not just about diet and activity. Three hormonal forces shape where fat sits and how stubborn it becomes: estrogen status, androgen excess, and cortisol load.
Before menopause, estrogen pushes fat storage toward the hips and thighs. The classic pear shape. As ovarian function declines through perimenopause and menopause, estrogen falls and fat redistributes toward the abdomen. The same woman who carried weight in her hips at 35 finds it parking around her waist at 50. This visceral shift is independent of total weight gain. Many women in menopause add only a few kilograms on the scale but lose two inches off their hips and gain three around the waist. The cardiovascular risk profile worsens even when the BMI barely moves.
In women of reproductive age, polycystic ovary syndrome (PCOS) is the dominant hormonal cause of central fat. Insulin resistance drives androgen production from the ovaries and adrenal glands, and the elevated androgens then push fat storage centrally. The 2023 international PCOS guideline places dietary modification, weight reduction, and consideration of insulin sensitisers as first-line therapy for women with elevated BMI and PCOS [Teede HJ et al. International PCOS Guideline 2023]. Cortisol from chronic stress and disturbed sleep adds a third layer, driving overnight glucose elevation and abdominal fat retention. The DermaVue protocol screens for all three. Fasting insulin, HOMA-IR, free testosterone, DHEA-S, and TSH are part of the baseline panel for any woman presenting with stubborn belly fat. Treatment then targets the dominant driver.
Belly Flab, Tummy Fat, Abs Fat: Glossary for Colloquial Terms
Patients describe belly fat in many ways. Doctors use a different vocabulary. This short glossary maps the everyday language to the clinical terms.
- Belly flab. Usually refers to soft, pinchable tissue at the lower abdomen. Clinically this is mostly subcutaneous fat. Lower metabolic risk than visceral fat but visible.
- Tummy fat. A general umbrella term that bundles both subcutaneous belly fat and visceral fat. Patients use it to describe a protruding waistline regardless of whether it is soft or firm.
- Abs fat. Fat that sits over the rectus abdominis and obscures the muscle definition underneath. This is again mostly subcutaneous fat. The visible six pack appears when this layer thins enough for the muscle to show through.
- Pot belly or paunch. A firm, protruding upper abdomen with a tight feel rather than soft fold. Almost always reflects high visceral fat. This is the metabolically dangerous pattern.
- Love handles. Fat over the iliac crest at the sides of the waist. Mostly subcutaneous. Cosmetic concern, lower metabolic concern.
- Mommy pooch. Lower abdominal softness after pregnancy. Often a mix of residual subcutaneous fat and rectus diastasis (separation of the abdominal muscles).
- Visceral fat. The clinical term. Fat stored deep in the abdomen around the liver, pancreas, and intestines. Cannot be pinched. Drives metabolic disease and is the target of medical treatment.
Generic GLP-1 Update. March 2026
Generic semaglutide entered the Indian market in March 2026. Branded Ozempic at 0.5 mg weekly previously ran around Rs 8,100 per month. Indian generics from Natco, Alkem, and Dr. Reddy's now sit between Rs 1,290 and Rs 4,200 at the same dose. The molecule and safety profile are identical. Physician supervision is still required because GLP-1 therapy carries real contraindications. Cheaper does not mean safer to self-prescribe.
Reviewed by Dr. Minu Liz Mathew, MD DVL · Last updated 5 April 2026
Frequently Asked Questions. Belly Fat Reduction
Reviewed by Dr. Minu Liz Mathew, MD DVLThe Condition
What causes belly fat in Indians even at normal weight?
The "Asian Indian Phenotype" causes preferential visceral fat storage due to genetic and dietary factors. Indians store more fat around organs even at normal BMI, making them metabolically unhealthy despite appearing thin. This is compounded by high refined carbohydrate diets and sedentary lifestyles common in urban India.
Can exercise alone reduce visceral belly fat?
Exercise helps but cannot specifically target visceral fat. Studies show GLP-1 therapy combined with resistance training is significantly more effective than exercise alone for visceral fat reduction. Cardio without strength training can actually worsen the problem by causing muscle loss.
How is visceral fat measured?
At DermaVue, we use waist circumference measurement and bioelectrical impedance analysis (BIA) to assess body composition. Waist circumference greater than 85 cm for men or 75 cm for women indicates high visceral fat risk in Indians. These thresholds are lower than Western standards because of our genetic predisposition.
The Treatment
How long does belly fat reduction take with GLP-1?
Most patients notice reduced appetite in week 1. Visible waist reduction typically occurs by month 3, with 5-8 cm lost from the waist. Significant visceral fat loss happens by month 6, with 10-16% total body weight reduction. By month 12, patients achieve 15-22% total weight loss with confirmed metabolic improvement.
Is this treatment safe for vegetarians?
Absolutely. Our clinical dietitian creates protein-optimized meal plans for vegetarians using paneer, dal, soya, Greek yogurt, and targeted supplements. Adequate protein intake (1.2-1.6g per kg body weight) is critical during GLP-1 therapy to preserve muscle mass, and this is fully achievable on a vegetarian diet.
What happens after I stop GLP-1 medication?
The SuperHuman program focuses on sustainable habit building during treatment. Protein optimization, resistance training routines, and balanced eating patterns are established during the treatment period so they become second nature. Most patients maintain their results because the program changes their relationship with food and exercise, not just the number on the scale.
Cost & Safety
What is the cost of belly fat treatment at DermaVue?
The belly fat reduction program starts at ₹5,660 per month for semaglutide and ₹13,000 per month for Mounjaro (tirzepatide). Costs include physician consultations, body composition analysis, and dietitian sessions. Generic GLP-1 medications are entering the Indian market. Pricing will be updated as new options become available.
Will I lose muscle mass on this program?
Without proper supervision, 25-45% of GLP-1 weight loss can be lean muscle. DermaVue's sarcopenia prevention protocol includes protein optimization (1.2-1.6g/kg), creatine supplementation, structured resistance training, and monthly grip strength monitoring to ensure you lose fat, not muscle.