Gynecomastia Surgery in Kerala | Male Chest Reduction
Evidence-based male breast reduction addressing glandular hypertrophy and pseudogynecomastia. Performed by board-certified MD DVL surgeons utilising precise excision and liposuction techniques in sterile, hospital-standard environments. 7 clinic locations across Kerala & Tamil Nadu.
What Is Gynecomastia?
Gynecomastia is a medical condition characterised by benign enlargement of male breast tissue due to fibroglandular proliferation, affecting an estimated 40–60% of Indian males at some stage of life. It must be clinically differentiated from pseudogynecomastia (pure fat accumulation) through diagnostic ultrasound. At DermaVue Kerala, treatment involves a mandatory hormonal workup followed by surgical excision of the glandular disc combined with peripheral liposuction for contour blending, performed under general anaesthesia by board-certified MD DVL surgeons. Reference: PubMed — Gynecomastia Epidemiology.
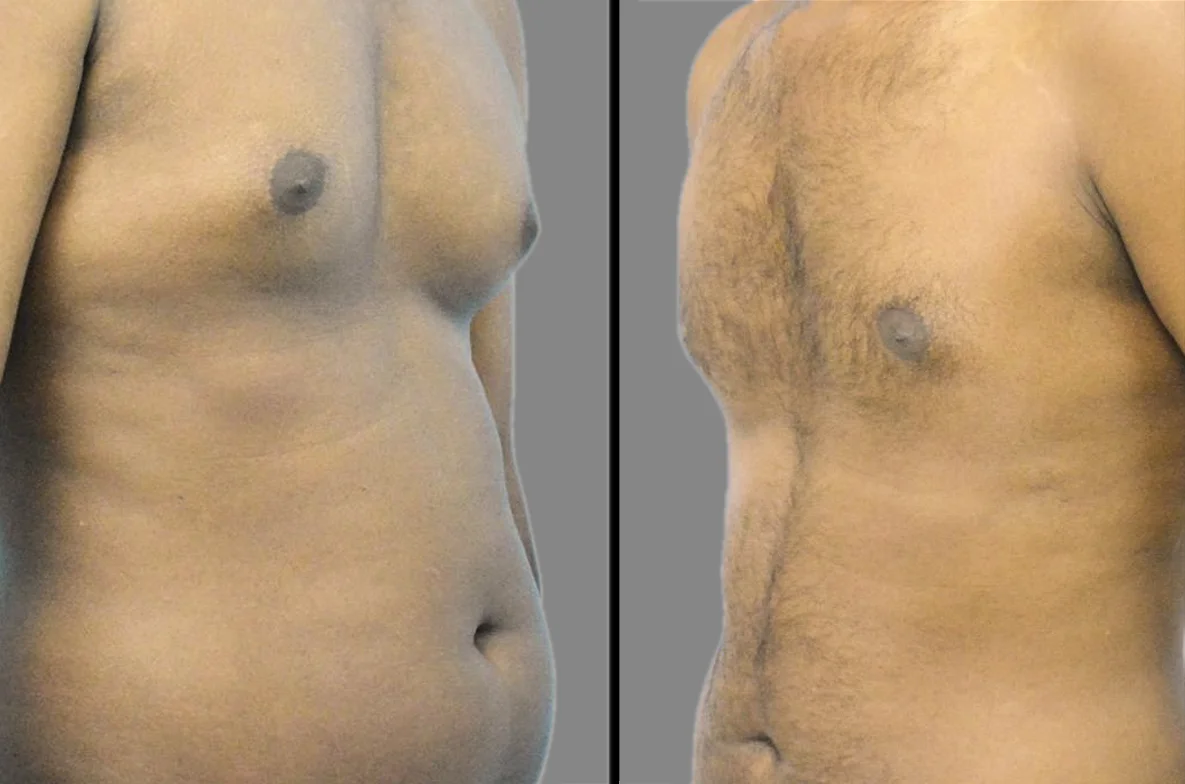
Gynecomastia: Causes, Diagnosis & Treatment
Gynecomastia is a medical condition characterised by the benign proliferation of fibroglandular tissue within the male breast. It must be clinically differentiated from pseudogynecomastia, which is merely the accumulation of adipose (fat) tissue without underlying glandular hypertrophy. In India, clinical data indicates a high prevalence, with an estimated 40% to 60% of males experiencing varying degrees during their lifetime.
The condition is primarily triggered by alterations in the estrogen-androgen ratio, which can occur naturally during neonatal development, puberty, or advancing age. However, in recent years, there has been a marked clinical increase in cases directly linked to the utilisation of anabolic steroids within gym culture, alongside idiopathic (unknown cause) presentations.
The psychological burden of gynecomastia is often substantial, leading to profound social stigma, altered posture, and psychological distress among young men. DermaVue addresses this condition comprehensively; prior to any surgical intervention, board-certified physicians conduct a thorough endocrinological evaluation to identify underlying hormonal, pharmacological, or systemic aetiologies. For patients with Fitzpatrick IV-VI skin types, surgical planning meticulously accounts for incision placement around the areolar border to minimise the risk of hypertrophic or keloid scarring.
Gynecomastia Types & Grades Treated at DermaVue
Surgical technique is directly dictated by the anatomical severity of the condition, universally categorised by the Simon Classification system.
Minor Enlargement
Minor breast enlargement strictly localised around the areola, lacking excess skin. Treated primarily through a small infra-areolar surgical excision to remove the glandular disc.
Moderate Enlargement
Moderate enlargement without (IIA) or with minor (IIB) skin excess. This common presentation frequently requires a combination of precise glandular excision and targeted ultrasonic or tumescent liposuction to seamlessly blend the chest contour into the surrounding musculature.
Significant Enlargement
Significant enlargement with pronounced ptosis (sagging skin) mimicking female breast tissue. Requires comprehensive tissue excision, extensive peripheral liposuction, and complex surgical skin resection (mastopexy) to restore a flat contour.
Who Is a Suitable Candidate for Gynecomastia Surgery?
Determining surgical candidacy involves both anatomical assessment and psychological readiness.
✓ Suitable Candidates
- Men with stable, fully developed glandular tissue present for more than 12 months
- Patients who have completely ceased use of anabolic steroids or offending medications
- Individuals with realistic expectations regarding peri-areolar scar placement
- Those experiencing physical discomfort (tenderness) or profound psychosocial distress
- Patients committed to 4–6 weeks of strict post-operative compression garment wear
✕ Not Yet Suitable
- Adolescents with transient pubertal gynecomastia (often resolves spontaneously)
- Active, unmanaged hormonal imbalances (e.g., hyperthyroidism, severe hypogonadism)
- Significant systemic obesity; requiring medical weight loss prior to chest contouring
- Heavy smokers unable to cease nicotine use prior to surgery, risking tissue necrosis
- Individuals with severe, unmanaged cardiovascular or pulmonary conditions
The DermaVue Gynecomastia Procedure
Integrating diagnostic diligence with precise surgical execution within an uncompromising hospital-standard OT setting.
Diagnostic Workup
Pre-operative hormonal profiling and high-resolution ultrasound imaging to definitively differentiate between lipomatous (fat) and fibroglandular dominance.
Anaesthesia
The 1-to-2-hour procedure administered under General Anaesthesia (GA) or deep sedation, monitored continuously by an experienced anaesthesiologist.
Liposuction Phase
If lipomatous tissue is present, tumescent fluid is infused and micro-cannulas aspirate fat to contour the peripheral chest wall, axilla, and lateral thorax seamlessly.
Excision Phase
A discrete peri-areolar incision extracts the dense, fibrotic glandular disc located directly beneath the nipple-areola complex.
Closure & Drains
Deep tissues approximated and sutured. In severe grades (III/IV), small surgical drains may be temporarily placed to prevent hematoma and seroma formation.
Discharge
Patients securely fitted into a specialised compression vest and typically discharged the same day following post-anaesthesia clearance and ambulation.
Gynecomastia Recovery Timeline
Adherence to postoperative limitations is critical to prevent hematoma and support skin retraction.
Initial Recovery
Mild to moderate soreness; drains (if utilised) typically removed at 48 hours. Maximum swelling occurs. Strict rest. Avoid raising arms above shoulder level to prevent pectoral tension.
Early Healing
Bruising transitions in colour. Sutures clinically evaluated. Compression vest must be worn continuously. Return to light desk work or academic studies. Light, unhurried walking permitted.
Primary Healing
Primary edema subsides. Nipple sensitivity may fluctuate (hyper/hypersensitivity). Resume lower body workouts. Absolute restriction on chest engagement.
Final Contouring
Deep tissue remodelling solidifies the final contour. Incision lines mature, soften, and fade. Return to unrestricted upper body weight training. Vest discontinued.
Gynecomastia Grade Assessment
Answer 3 questions about your condition to receive an estimated clinical grade and expected surgical approach.
Expected Results from Gynecomastia Surgery
Once the mature fibroglandular tissue is surgically excised, the results are typically considered permanent, provided the patient avoids exogenous androgens, anabolic steroids, or specific pharmacological agents that induce glandular hypertrophy. Most patients experience a significantly flattened, well-contoured masculine chest profile. Skin retraction over the newly flattened chest takes several months to optimise fully. Minor, transient asymmetry is a natural occurrence during the swelling phase. Changes in nipple sensation frequently resolve within the first six to twelve months post-operatively.
DermaVue vs. Other Providers for Gynecomastia
| Feature | DermaVue | Technician Clinic | General Salon |
|---|---|---|---|
| Pre-Op Hormonal Workup | ✓ Mandatory Endocrine Panel | ✕ Skipped / Optional | ✕ None |
| Surgeon Qualification | ✓ Board-Certified MD DVL | ✕ General Practitioner | ✕ Non-Medical Staff |
| Dual-Modality Technique | ✓ Lipo + Excision Combined | ✕ Lipo Only (Incomplete) | ✕ Not Available |
| Facility Standard | ✓ Hospital-Standard OT | ✕ Clinic Room | ✕ Non-Certified |
| Saucerisation Prevention | ✓ Precise Disc Removal | ✕ Over-Resection Risk | ✕ Not Applicable |
| Steroid-Induced Cases | ✓ Specialised Experience | ✕ Limited | ✕ None |
| Patient Reviews | ✓ 4.8★ — 7,200+ Verified | ✕ Few Reviews | ✕ Unverified |
Gynecomastia Surgery Cost in Kerala
Transparent Pricing at DermaVue
This variance is strictly tied to the Simon’s Grade of the condition. Grade I procedures requiring minor, localised excision are at the lower end. Conversely, Grade III or IV interventions necessitating extended surgical time, combined multi-zone liposuction, complex skin resection, and prolonged anaesthesia reside at the upper threshold.
The comprehensive fee includes the surgeon’s execution, the anaesthesiologist, and the utilisation of a hospital-standard operating facility.
Gynecomastia Surgery for NRI & Gulf Patients
Discreet Medical Care During Annual Leave
A substantial percentage of our patient demographic includes young professionals travelling from the UAE, Saudi Arabia, Oman, and the broader Gulf region during their annual leave to address this condition discreetly away from their professional environments.
DermaVue facilitates this specific medical tourism by offering detailed pre-arrival tele-consultations for grade assessment and coordinating all necessary medical documentation. The clinical pathway is structured to ensure that surgical drains (if required) are removed and initial healing is stabilised within a typical 10-to-14-day travel window prior to flying back.
Why DermaVue for Gynecomastia
Comprehensive Diagnostics
Board-certified MD DVL physicians mandate proper endocrinological assessment to rule out pathological systemic causes before proposing surgery.
Dual-Modality Technique
Mastery in combining advanced liposuction with direct glandular excision to prevent “saucerisation” (an unnatural, dished-out appearance behind the nipple).
Hospital-Standard Safety
Procedures performed in strict sterile OT environments, actively rejecting the severe risks associated with non-accredited cosmetic salons.
Steroid-Case Expertise
Extensive institutional experience managing both idiopathic cases and complex, dense steroid-induced gynecomastia common in modern fitness demographics.
About Gynecomastia Surgery at DermaVue
DermaVue is a physician-owned dermatology and plastic surgery network operating 7 clinics across Kerala and Tamil Nadu, India, offering comprehensive gynecomastia correction under board-certified MD DVL surgeons in hospital-standard operating theatres. The network mandates pre-operative endocrinological evaluation before any surgical intervention, employing a dual-modality approach combining precise glandular excision with peripheral liposuction for optimal male chest contouring. With a 4.8-star aggregate rating from over 7,200 verified Google reviews, DermaVue is a preferred destination for NRI and Gulf patients seeking discreet, evidence-based gynecomastia surgery during annual leave, with clinics in Thiruvananthapuram, Kollam, Thiruvalla, Kottayam, Kochi, Thrissur, and Coimbatore. References: PubMed — Gynecomastia Surgical Outcomes, NIH — Simon Classification System.
Meet Your Gynecomastia Surgeons
Every gynecomastia procedure at DermaVue includes mandatory hormonal workup and is performed by board-certified specialists.
Co-founder and Managing Director of DermaVue, Dr. Sarath Chandran brings extensive experience in male chest contouring. His dual-modality approach ensures complete glandular disc removal combined with precise peripheral liposuction, preventing saucerisation while achieving a naturally flat masculine contour. Specialises in complex steroid-induced cases.
Dr. Minu Liz Mathew brings meticulous surgical precision to gynecomastia correction with particular expertise in minimising peri-areolar scarring in melanin-rich skin types. Her diagnostic approach ensures comprehensive hormonal evaluation before any surgical intervention, and her UAL technique delivers seamless contour blending in Grade IIA/IIB cases.
Gynecomastia Surgery FAQs
Is gynecomastia surgery safe in Kerala?
What is the recovery time after gynecomastia surgery?
Is gynecomastia surgery painful? What anaesthesia is used?
How much does gynecomastia surgery cost in Kerala?
Who performs gynecomastia surgery at DermaVue?
How many sessions are needed for gynecomastia correction?
Can gynecomastia surgery be combined with other treatments?
When will I see results after gynecomastia surgery?
What happens if I have pseudogynecomastia?
Will the tissue grow back if I use steroids?
Ready for a Flat, Confident Chest?
Our board-certified surgeons at DermaVue specialise in comprehensive gynecomastia correction with mandatory hormonal workup, dual-modality surgical technique, and hospital-standard safety. Join 7,200+ patients who trust DermaVue across Kerala & Tamil Nadu.