Dandruff Treatment in Thiruvalla
Expert Scalp Care & Seborrheic Dermatitis Solutions
Dandruff not responding to shampoos? It may be seborrheic dermatitis — a medical condition. DermaVue offers lasting scalp solutions beyond OTC treatments.
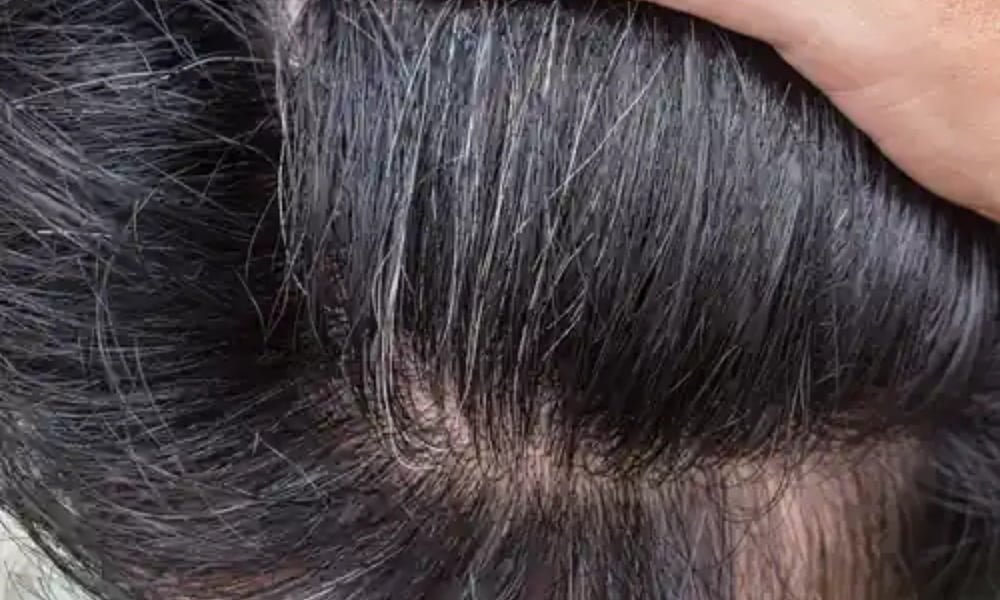
Understanding Seborrheic Dermatitis: Malassezia Biology & Proper Medical Therapy
Quick Answer
Medical dandruff treatment in Thiruvalla/Tiruvalla targets Malassezia globosa and Malassezia restricta — the two lipophilic yeast species most associated with seborrheic dermatitis — with prescription ketoconazole 2% or ciclopirox olamine 1% shampoo (3–5 minute contact time, 2–3 times weekly), selenium sulphide 2.5%, zinc pyrithione, and topical calcineurin inhibitors (pimecrolimus, tacrolimus) for facial involvement. Recalcitrant disease is managed with oral itraconazole 200 mg daily pulse therapy. Differential includes scalp psoriasis, tinea capitis, and contact dermatitis.
DermaVue Clinical Summary — Seborrheic Dermatitis
Seborrheic dermatitis is a chronic relapsing inflammatory dermatosis of sebaceous-rich areas driven by an abnormal host response to commensal lipophilic yeasts of the genus Malassezia. Historical texts attributed the condition to Malassezia furfur, but modern molecular speciation has identified Malassezia globosa and Malassezia restricta as the dominant species on affected scalps — a speciation update reflected in the current IADVL and European S3 dandruff guidelines (Gaitanis et al., Clinical Microbiology Reviews 2012). These lipid-dependent yeasts hydrolyse sebum triglycerides to produce irritant free fatty acids and lipoperoxides, triggering the scaling, erythema and pruritus seen clinically.
Clinical presentations at DermaVue Thiruvalla span simple pityriasis capitis (non-inflammatory scalp flaking), classic scalp seborrheic dermatitis with erythema and greasy yellow scale, facial seborrheic dermatitis involving eyebrows, nasolabial folds, and retroauricular areas, infantile seborrheic dermatitis (cradle cap), and Malassezia folliculitis of the trunk (often misdiagnosed as acne). Important associations include Parkinson's disease, HIV infection (where disease is unusually severe and extensive), and immunosuppression — conditions screened for when clinically indicated. Differential diagnosis is critical: scalp psoriasis, tinea capitis, contact dermatitis, and atopic dermatitis can all mimic seborrheic dermatitis and have entirely different treatments.
First-line treatment follows the AAD and IADVL consensus (Naldi & Rebora, NEJM 2009; Dall'Oglio et al., JEADV 2022): ketoconazole 2% shampoo or ciclopirox olamine 1% shampoo used 2–3 times weekly with a minimum 3–5 minute scalp contact time before rinsing — compliance with contact time is the most common reason for "shampoo failure". Adjunctive options include zinc pyrithione 1–2% shampoo, selenium sulphide 2.5% lotion/shampoo, salicylic acid-coal tar shampoos for thick scale, and topical corticosteroid solutions (clobetasol, betamethasone) for inflamed flares — used short-course only. Topical calcineurin inhibitors (pimecrolimus 1% cream, tacrolimus 0.1% ointment) are preferred for facial involvement to avoid steroid-induced rosacea and telangiectasia. For severe or recalcitrant disease, oral itraconazole 200 mg daily for 7 days followed by pulse maintenance is an evidence-supported option (Kose et al., Mycoses 2005). Sources: IADVL, IJDVL, AAD, NEJM, PubMed, NIH MedlinePlus.
- Simple dandruff (pityriasis capitis) — scalp flaking only
- Seborrheic dermatitis — scalp, face, eyebrows, nasolabial folds, chest
- Dandruff with hair fall — Malassezia-induced follicular inflammation
- Scalp psoriasis — can mimic severe dandruff
- Cradle cap (infantile seborrheic dermatitis)
Understanding Seborrheic Dermatitis & Dandruff
Medical Dandruff Treatments at DermaVue Thiruvalla
When standard anti-dandruff shampoos fail, prescription-strength treatments and scalp procedures deliver lasting results. We match treatment to your scalp condition and severity.
- Prescription antifungal shampoos: ketoconazole 2%, selenium sulphide, ciclopirox
- Topical corticosteroid solutions and sprays for scalp inflammation
- Medicated scalp serums and lightweight lotions
- Scalp peeling with salicylic acid and lactic acid to remove scale
- Oral antifungals for severe or recalcitrant seborrheic dermatitis
- PRP or GFC therapy for dandruff-induced hair loss
- Seborrheic dermatitis face management
Ready to Book Your Dandruff Treatment in Thiruvalla?
DermaVue Thiruvalla — Iykara Peniel Tower, Opposite Indian Overseas Bank, Thukalassery. Mon–Sat 9 AM–7 PM, Sun 10 AM–6 PM.
Comprehensive Scalp Treatment for Dandruff
Frequently Asked Questions
Book Your Consultation at DermaVue Thiruvalla
Board-certified dermatologists. Hospital-standard OT. US-FDA approved equipment. Physician-led care — not technician-run.
What Our Patients Say
Real experiences from patients across our 7 clinics.
Visited this clinic for my skin concerns, and I'm extremely satisfied with the treatment. The doctor is knowledgeable and patient.
The skin treatment at DermaVue was excellent. The consultation was detailed, and the treatment plan was explained thoroughly.
Best dermatology clinic I've been to. The facilities are world-class and the results from my laser treatment exceeded expectations.
Visit Us at Any of Our 7 Clinics
Internationally certified dermatology care across Kerala and Tamil Nadu.