Melasma Treatment in Thiruvalla
Expert Pigmentation & Dark Spot Removal
High year-round UV exposure drives stubborn melasma. DermaVue treats the root cause with Q-switched laser, combination peels, and protocols tailored for South Indian skin.
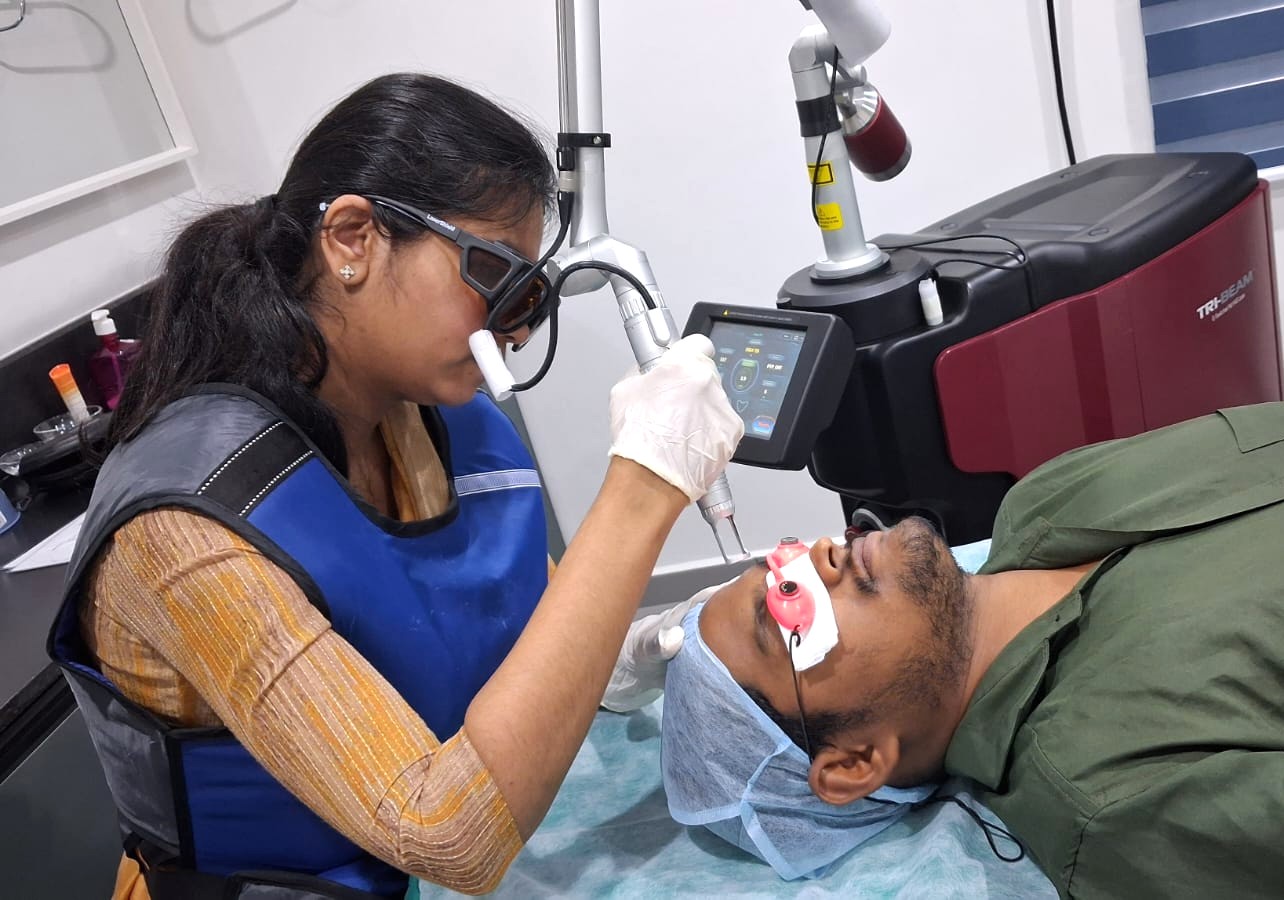
Understanding Melasma: Pathophysiology, Classification & Kerala Climate
Quick Answer
Melasma treatment in Thiruvalla/Tiruvalla follows the Pigmentary Disorders Academy protocol: Wood lamp classification (epidermal, dermal, mixed), modified Kligman trio (hydroquinone 4% + tretinoin 0.025% + hydrocortisone) as first-line, oral tranexamic acid 250 mg twice daily for resistant cases (with contraindication screening), low-fluence Q-switched Nd:YAG 1064 nm toning over 6–10 sessions, and daily iron-oxide tinted sunscreen SPF 50+ PA++++ to block visible light. Treatment is long-term; sun protection is non-negotiable.
DermaVue Clinical Summary — Melasma
Melasma is an acquired chronic symmetrical hypermelanosis of sun-exposed skin, characterised histologically by increased melanogenesis in the epidermis and, in dermal variants, by melanin-laden macrophages within the papillary dermis. The condition disproportionately affects Fitzpatrick skin types III–V — the predominant phototype across South India — with a strong female predominance and associations with pregnancy, combined oral contraceptives, thyroid dysfunction, and cumulative ultraviolet and visible-light exposure (Passeron & Picardo, Pigment Cell & Melanoma Research 2018). Kerala's near-equatorial latitude, year-round high UV index, and increasing visible-light exposure from digital devices together make melasma one of the most common pigmentary presentations at DermaVue Thiruvalla.
Clinical evaluation begins with Wood's lamp examination to classify melasma as epidermal (enhanced contrast under Wood's light — best prognosis), dermal (no contrast enhancement — poorest prognosis), or mixed. Severity is documented using the Melasma Area and Severity Index (MASI) and modified MASI (mMASI) for reproducible response tracking. Treatment follows the IADVL Pigmentary Disorders consensus (IJDVL 2017): topical modified Kligman trio (hydroquinone 4% + tretinoin 0.025% + hydrocortisone 1%) as standard first-line, azelaic acid 20%, cysteamine 5% cream, topical tranexamic acid 5%, and kojic acid-arbutin combinations as adjuncts.
For refractory or dermal melasma, DermaVue prescribes oral tranexamic acid 250 mg twice daily for 8–12 weeks (Bala et al., JAAD 2018; Del Rosario et al., JAAD 2018) after screening for contraindications including personal or family history of deep vein thrombosis, pulmonary embolism, stroke, active malignancy, pregnancy, or concurrent combined oral contraceptive use. Procedural adjuncts include low-fluence Q-switched Nd:YAG 1064 nm laser toning (6–10 sessions, 2–4 weeks apart), modified Jessner peels, mandelic acid 20–40% peels, and TCA 15–20% spot peels — each selected by depth and Fitzpatrick type. Critically, daily broad-spectrum iron-oxide tinted sunscreen SPF 50+ PA++++ is prescribed to block both UVA/UVB and high-energy visible (HEV) light — the single most outcome-defining step in every protocol (Dumbuya et al., JDD 2020). Sources: IADVL (iadvl.org), IJDVL, AAD, PubMed, NIH.
- Epidermal melasma — enhanced border contrast under Wood's lamp; best prognosis; responds to topical and superficial procedural therapy
- Dermal melasma — no contrast under Wood's lamp; dermal melanophages; most resistant; requires combination systemic-procedural approach
- Mixed melasma — features of both; commonest presentation in Kerala women
- Centrofacial pattern — forehead, nose, upper lip, chin; most common distribution
- Malar pattern — cheeks and nose
- Mandibular pattern — along the ramus of the mandible; associated with photoageing
- Post-inflammatory hyperpigmentation — following acne, eczema, or procedural injury
- Solar lentigines, ephelides and drug-induced pigmentation — differentiated clinically and by dermoscopy
Understanding Melasma & Pigmentation Causes
DermaVue Thiruvalla Combination Melasma Protocol
Melasma is chronic and relapse-prone; monotherapy rarely produces durable results. DermaVue follows a structured stepwise combination approach guided by Wood's lamp depth classification, Fitzpatrick type, pregnancy status, and prior therapy history. Treatment response is documented with serial mMASI scoring and standardised photography every 4 weeks.
- Modified Kligman trio (hydroquinone 4% + tretinoin 0.025% + hydrocortisone 1%) — first-line, 8–12 weeks, then pulsed maintenance
- Oral tranexamic acid 250 mg BD × 8–12 weeks — after contraindication screening (DVT/PE/stroke/malignancy/pregnancy/COC)
- Topical adjuncts: azelaic acid 20%, cysteamine 5%, topical tranexamic acid 5%, kojic acid-arbutin combinations, thiamidol
- Low-fluence Q-switched Nd:YAG 1064 nm laser toning — 6–10 sessions, 2–4 weeks apart; dermal and mixed melasma
- Superficial chemical peels: modified Jessner, mandelic acid 20–40%, TCA 15% spot peels — Fitzpatrick-adjusted
- Iron-oxide tinted mineral sunscreen SPF 50+ PA++++ — blocks UVA/UVB and visible light; reapplied every 2–3 hours; non-negotiable
- Hormonal review: thyroid function, OCP rationalisation, post-pregnancy timing counselling
- Maintenance phase: azelaic acid or tretinoin monotherapy, tranexamic acid pulse, quarterly Q-switched toning to prevent relapse
Ready to Book Your Melasma Treatment in Thiruvalla?
DermaVue Thiruvalla — Iykara Peniel Tower, Opposite Indian Overseas Bank, Thukalassery. Mon–Sat 9 AM–7 PM, Sun 10 AM–6 PM.
Comprehensive Pigmentation Treatment Guide
Frequently Asked Questions
Book Your Consultation at DermaVue Thiruvalla
Board-certified dermatologists. Hospital-standard OT. US-FDA approved equipment. Physician-led care — not technician-run.
What Our Patients Say
Real experiences from patients across our 7 clinics.
Visited this clinic for my skin concerns, and I'm extremely satisfied with the treatment. The doctor is knowledgeable and patient.
The skin treatment at DermaVue was excellent. The consultation was detailed, and the treatment plan was explained thoroughly.
Best dermatology clinic I've been to. The facilities are world-class and the results from my laser treatment exceeded expectations.
Visit Us at Any of Our 7 Clinics
Internationally certified dermatology care across Kerala and Tamil Nadu.